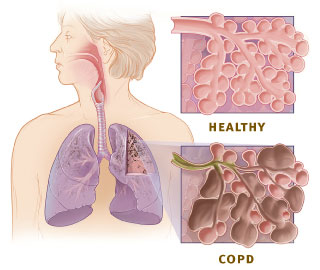
Understanding Chronic Bronchitis: A Multifactorial Challenge
Chronic bronchitis, a debilitating respiratory condition, is characterized by a persistent cough with mucus production for at least three months in two consecutive years, often in the absence of other specific lung diseases. Unlike acute bronchitis, which typically resolves, chronic bronchitis involves sustained inflammation and irritation within the bronchial tubes. Its precise origins remain under scientific investigation, yet it's clear that a complex interplay of both external (exogenous) and internal (endogenous) factors drives its development. Central to this understanding is the concept of an Exogene Infektion – external infections and environmental influences originating from outside the body. These exogenous factors frequently initiate the inflammatory processes that lead to chronic airway changes.
The Dominance of Exogenous Infections and Environmental Irritants
When considering chronic bronchitis, the role of Exogene Infektionen and environmental pollutants is paramount. These external agents continuously challenge our respiratory system, transforming acute inflammation into a chronic state through recurrence or persistence.
Viral and Bacterial Invaders
Acute infections, particularly those caused by Mycoviruses and specific bacteria, are identified as key precursors. What starts as a common cold can, especially with compromised immunity or repeated exposure, escalate into persistent bronchial irritation. These infections compromise the respiratory lining, making it vulnerable to secondary bacterial infections, thus exacerbating inflammation and mucus production. The immune response, while fighting pathogens, contributes to long-term tissue damage and remodeling within the airways, setting the stage for chronic symptoms. Repeated infectious Exogene Infektionen are a significant pathway to chronic respiratory conditions.
Particulate Matter and Noxious Gases
Beyond microbes, our environment exposes us to non-biological irritants. Industrial dust, chemical gases, and particulate matter from smog and vehicle emissions are potent exogenous factors. These compounds directly irritate the bronchial lining, triggering a sustained inflammatory response. Prolonged inhalation leads to continuous tissue damage and repair cycles, altering airway structure and function. While nitrogen acid and general allergens play a secondary role, their cumulative contribution to the inflammatory burden can still enhance chronic disease risk. For a deeper dive into these external triggers, read our article: Unraveling Exogenous Factors: Key Triggers of Chronic Bronchitis.
Fluor's Potent Role in Smog-Induced Bronchitis
Among environmental pollutants, Fluor's impact merits critical attention. Our reference context highlights Fluor as a "most important factor," especially in smog. The tragic Meuse Valley disaster, where severe air pollution caused acute respiratory illnesses and deaths, stands as a stark reminder. Competent authors then specifically implicated Fluor as a significant contributor.
Fluor compounds, notably hydrogen fluoride (HF) and silicon tetrafluoride (SiF4), are highly corrosive gases. Inhaled, they inflict severe irritation and damage upon the delicate respiratory tissues. HF, particularly, is known for rapid tissue penetration, causing deep, persistent inflammation and even necrosis. In chronic bronchitis, sustained exposure to Fluor-containing smogs directly contributes to chronic inflammation, excessive mucus secretion (bronchorrhoea), and structural remodeling. Such powerful chemical irritants in the air constitute a profound Exogene Infektion of the respiratory system, demanding heightened public health vigilance and stringent regulatory measures. For more on the interconnectedness of environmental factors, explore: Exogenous Infections & Smog: Dominant Factors in Chronic Bronchitis.
Beyond External Triggers: Exploring Endogenous Influences
While external factors, especially Exogene Infektionen and pollutants, are primary drivers, chronic bronchitis is also shaped by internal, or endogenous, influences. These intrinsic predispositions can increase susceptibility to external triggers or directly contribute to airway pathology.
Hormonal Imbalances and Exudative Diathesis
Hormonal influences, particularly involving the adrenal glands, are an area of interest. A relative adrenal insufficiency, reducing corticosteroid production, has been proposed as a cause of chronic bronchorrhoea. Corticosteroids regulate inflammation; their deficiency could lead to uncontrolled bronchial inflammation, potentially manifesting as an 'exudative diathesis'—a predisposition to inflammatory exudates. This suggests an intricate interplay where endogenous hormonal imbalance might amplify external irritants or initiate a chronic secretory process.
Hereditary and Genetic Factors
Genetic predispositions, though less common, play a role. Inherited conditions like mucopolysaccharide defects, alpha-1 antitrypsin deficiency, and immunoglobulin deficiencies increase susceptibility to chronic respiratory issues. Alpha-1 antitrypsin deficiency, for instance, impairs elastic lung tissue protection, raising COPD risk. Immune deficiencies can make individuals more vulnerable to recurrent Exogene Infektionen, perpetuating inflammation.
Nervous and Allergic Components
General nervous and psychological factors are typically minor in primary chronic bronchitis pathogenesis but can affect overall health. Allergic diatheses, however, can contribute to airway hyperresponsiveness and inflammation, especially where chronic bronchitis symptoms overlap with allergic asthma. Nevertheless, for chronic bronchitis specifically, allergies usually play a secondary or exacerbating role compared to infections and environmental pollutants.
Mitigating Risk: Practical Strategies for Prevention and Management
Given the multifactorial nature of chronic bronchitis, with its heavy reliance on Exogene Infektionen and environmental pollutants, a comprehensive, proactive approach to prevention and management is paramount. Implementing the following strategies can significantly reduce risk and improve quality of life:
- Minimize Exposure to Pollutants:
- Smoking Cessation: The most impactful step. Avoid all tobacco smoke.
- Air Quality Awareness: Monitor local indexes. Limit outdoor activity on high pollution days.
- Indoor Air Quality: Use HEPA air purifiers; ensure good ventilation.
- Occupational Safety: Use PPE (respirators) and ensure ventilation if exposed to dust, chemicals (Fluor compounds) at work.
- Prevent and Manage Infections:
- Vaccination: Stay updated with influenza and pneumococcal vaccines.
- Rigorous Hygiene: Practice frequent hand washing.
- Avoid Crowds: Minimize exposure during peak cold/flu seasons to reduce viral Exogene Infektionen.
- Prompt Medical Attention: Seek timely care for acute respiratory infections to prevent chronicity or complications.
- Support Overall Respiratory Health:
- Hydration: Drink plenty of fluids to thin mucus.
- Nutrient-Rich Diet: Consume antioxidants and anti-inflammatory foods.
- Regular, Safe Exercise: Exercise in good air quality to improve lung capacity.
- Collaborative Medical Management: Work with healthcare professionals for personalized plans, including medications and addressing endogenous factors.
Conclusion
Chronic bronchitis is a formidable respiratory challenge, profoundly influenced by Exogene Infektionen and environmental irritants, notably Fluor in smog. While endogenous factors shape individual susceptibility, the external environment provides the initial and ongoing insults. A holistic approach—integrating rigorous environmental protection, proactive infection prevention, and personalized medical management—offers the best pathway to mitigate this condition's incidence and severity. Ongoing research continues to unravel its intricate mechanisms, promising more targeted and effective interventions to improve global quality of life.